 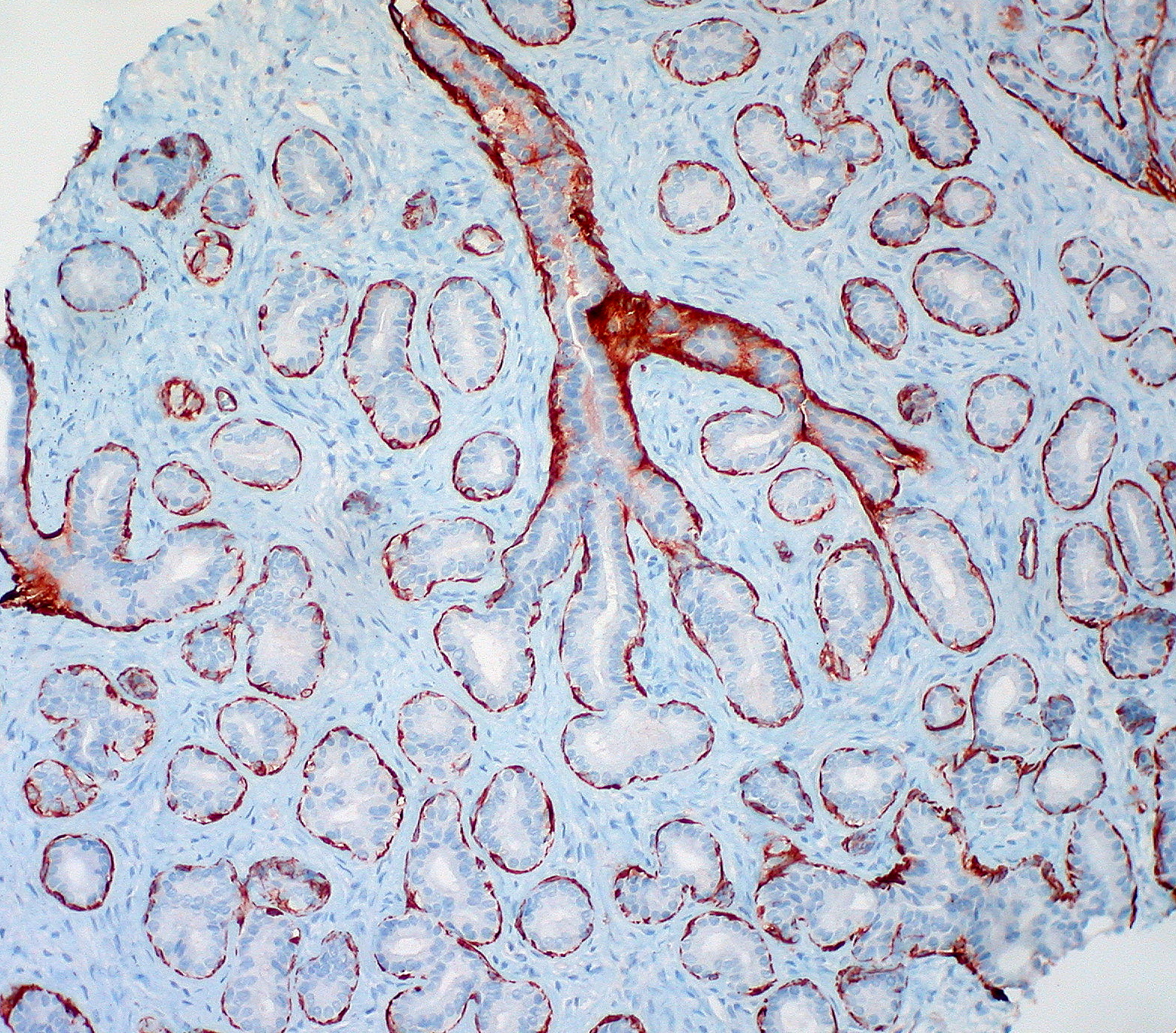
It is now believed that specific subsets of serrated polyps account for over 30% of colorectal cancers (CRCs). The identification of this lesion, now called a traditional serrated adenoma (TSA), helped lead to a careful re-evaluation of the entire class of serrated colonic polyps by Torlakovic et al. In the 1990s, Longacre and Fenoglo-Preiser et al coined the term “serrated adenoma” to describe a class of polyps that “exhibited the architectural but not the cytologic features of a hyperplastic polyp”. Prior to the 1990s, essentially all serrated polyps were called hyperplastic polyps (HP) and it was thought these lesions had no potential for malignancy. 
Within the last 2 decades, our knowledge of colorectal SSPs has transformed dramatically and it has led to marked changes in the terminology used to describe the spectrum of serrated polyps. These lesions should be on the endoscopists’ most wanted list. There is no wonder that there is a need to understand these lesions well, learn how best to prevent the colonic mucosa from going down this errant path or, if that fails, to detect these deviants and eradicate them from colonic society. As will be described, these lesions have multiple aliases (serrated adenoma, serrated polyp or serrated lesion among others), they hang out in a bad neighborhood (the poorly prepped right colon), they hide behind a mask of mucus, they are difficult for witnesses (pathologists) to identify, they are difficult for police (endoscopists) to find, they are difficult to permanently remove from society (high incomplete resection rate), they can be impulsive (progress rapidly to CRC) and enforcers (gastroenterologists) don’t know how best to control them (uncertain surveillance recommendations). Colorectal cancer risk factors.The sessile serrated polyp (SSP), also known as sessile serrated adenoma, is the evil twin among the colorectal cancer precursors. Surveillance of colonic polyps: are we getting it right? World J Gastroenterol. State insurance mandates and the ACA essential benefits provisions.īonnington SN, Rutter MD. National Conference of State Legislatures. Understanding your pathology report: colon polyps (sessile or traditional serrated adenomas). Association between adenoma location and risk of recurrence. Understanding polyps and their treatment. doi: 10.1001/jama.2021.6238.Īmerican Society for Gastrointestinal Endoscopy. Screening for colorectal cancer: US Preventive Services Task Force recommendation statement. ACG clinical guidelines: colorectal cancer screening 2021. Shaukat A, Kahi CJ, Burke CA, Rabeneck L, Sauer BG, Rex DK. Colorectal adenoma to carcinoma progression is accompanied by changes in gene expression associated with ageing, chromosomal instability, and fatty acid metabolism. Colorectal cancer screening: an updated review of the available options. Characteristics of and risk factors for colorectal neoplasms in young adults in a screening population. Lee SE, Jo HB, Kwack WG, Jeong YJ, Yoon YJ, Kang HW. Mutation analysis of adenomas and carcinomas of the colon: early and late drivers. Adenomatous polyposis syndromes: diagnosis and management. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
